Sleep architecture changes
Sleep architecture changes
Sleep architecture on a polyphasic schedule is potentially different from a monophasic schedule. Let’s find out!
This section will focus on how the overall sleep architecture changes when people adapt to a polyphasic schedule.
Background
At this point in time, reducing SWS or REM sleep leads to several negative consequences.
- SWS is the sleep stage where the glymphatic system is most active. In addition, it also repairs damaged cells.
- SWS is also responsible for long-term memory consolidation.
- REM sleep is responsible for several types of memory consolidation. Examples include procedural, spatial and emotional memory formation.
- Reducing these sleep stages triggers the feelings of sleep deprivation.
- Consistently reducing them for a long time can result in immune system deficiency, obesity, cardiovascular diseases, diabetes, etc.
Both of these sleep stages are, because of this, vital sleep stages. What that means is that they serve vital functions for the body; reducing them leads to sleep deprivation and can really harm the body. When you miss out on sleep, the body will attempt to partially salvage the missed out SWS and REM sleep during the recovery. However, the same doesn’t happen with light sleep.
Current situation
After establishing that reducing SWS or REM sleep leads to negative consequences, what is the situation with polyphasic sleepers?
Well, the community has been working on the “EEG labeling project”. Some community members who attempt polyphasic schedules are interested in tracking their sleep stages so that they can see how their adaptations progress.
This data is then collected and processed to determine exactly how the sleep architecture will change after adaptation. The project is still ongoing; however, there are already some quite nice-looking readings for you to see.
Everyman 1
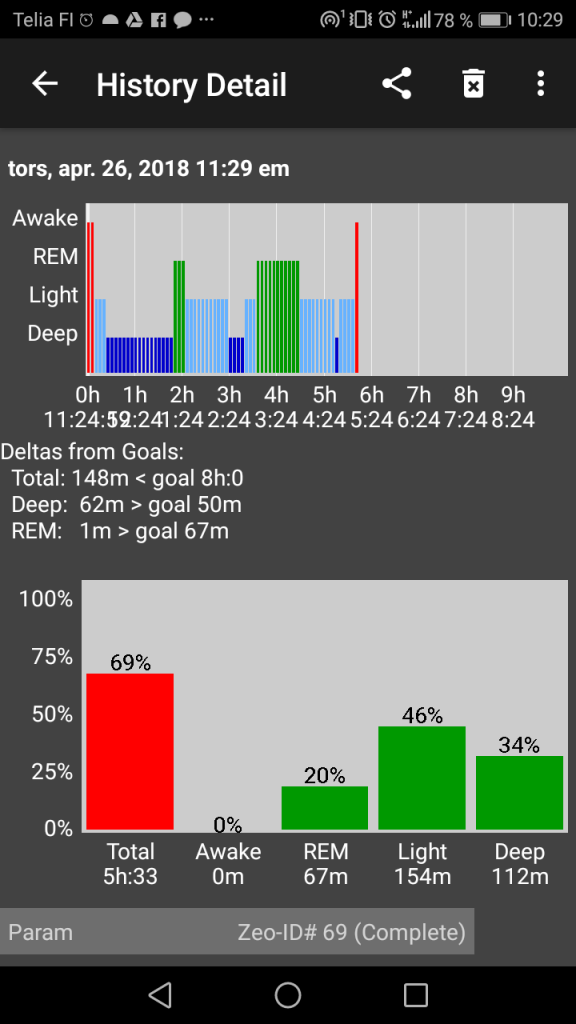
This picture is an EEG reading from Crimson when he just started attempting the Everyman 1 schedule. After he had adapted to the schedule, this is one of the readings he got:
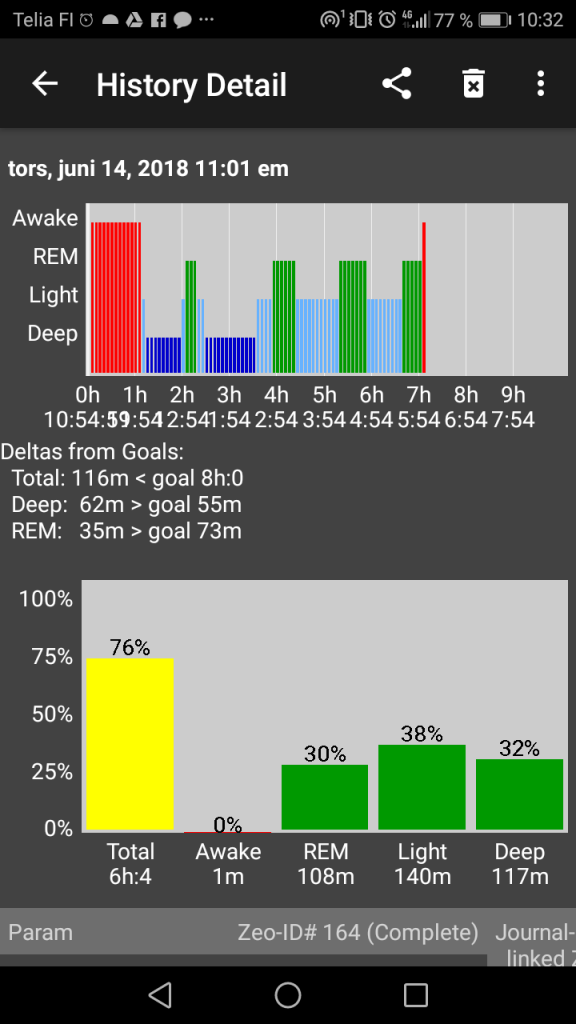
- The amount of SWS that he had stayed relatively consistent.
- The duration of REM sleep increased significantly at the expense of light sleep.
- This also matched with his monophasic sleep requirements; thus, he was able to get all needed SWS and REM sleep from the schedule.
Everyman 2-extended
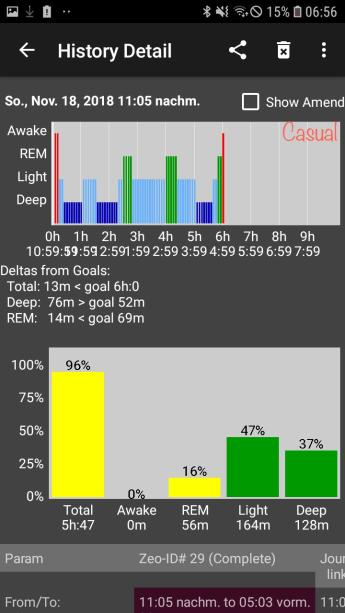
Another good hypnogram we can look at is from Feili. First, I want to tell you that his baseline monophasic requirements were around 90 minutes of REM sleep and 130 minutes of SWS.
When he started his schedule, he clearly got less REM sleep than what he needed. However, after adapting, you can see that his REM has increased to account for almost all his needs. The remaining REM amount comes from his naps:
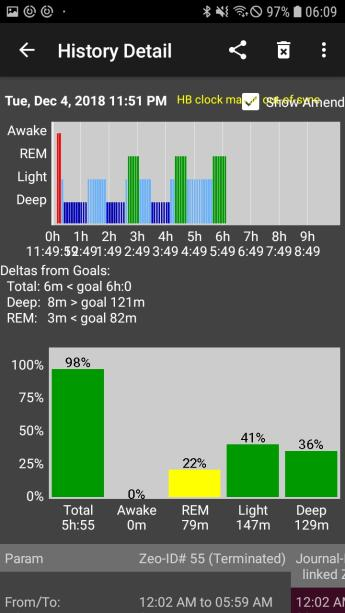
This picture is actually from his morning nap, which was almost overflowing with REM:
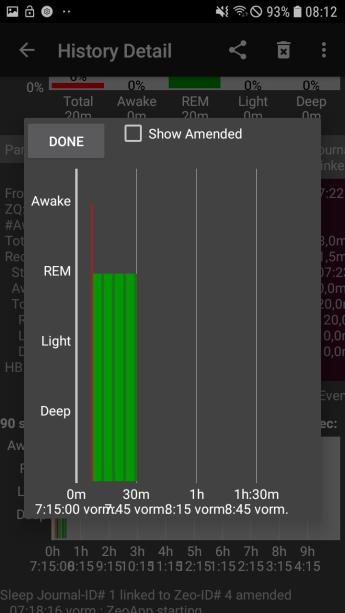
The future
In the future, the EEG labeling project is going to continue. Evidence for whether this repartitioning happens for several people or only a select few will also undergo assessment. So far, it seems like repartitioning is something that happens for many people.
If you have EEG readings from before and after you started a polyphasic schedule, share with us. Reach us over the Discord, even if your readings show that you get different amounts. That way, we can further this community’s understanding of sleep architecture in general, and polyphasic schedules in particular.
Changes in Light sleep architecture
Light sleep reduction
What does reducing light sleep entail? After adapting to a polyphasic schedule, the same duration of SWS and REM sleep should be obtainable as when people are monophasic. But what happens to light sleep? First, light sleep is definitely going to reduce after adapting to a polyphasic sleep schedule. This is except the case of non-reducing polyphasic schedules.
- During an adaptation, the body is going through several different defense mechanisms. This is to ensure that it gets the required amount of SWS and REM sleep. In the meantime, there will be some sacrifice of light sleep.
- The fact that this happens is somewhat telling about how the body treats light sleep; it looks like a sort of filler type of sleep.
- Furthermore, light sleep does not really build any type of sleep pressure.
- When you are missing out on SWS or REM sleep, your body is going to want to get more of these. Eventually, your body will insert the sleep type very early in each sleep session. These terms are SOREM and SOSWS to protect the necessary durations of these sleep stages.
Light sleep recovery
However, this is not a mechanism that happens with light sleep. When you get less light sleep, your body makes absolutely no effort to recover more of it. In addition, this is a perfect opportunity to point out that when you have sleep deprived yourself, your body is not going to catch up on light sleep. However, it does catch up with SWS and REM sleep.
- When you miss out on sleep, your body is going to sleep extra to recover around 70% of missed SWS and around 50% of missed REM sleep.
- However, it only recovers only 7% of missed light sleep, which supports the idea that it is a non-vital sleep stage.
Nevertheless, light sleep does serve some functions. However, there does not seem to be any VITAL functions associated with it.
- It helps with a bit of memory consolidation, especially memories related to movements (e.g, learning how to ride a bike). However, it’s not anything vital.
- Light sleep is also responsible for acting as a wakefulness sustainer; this is one of the reasons why we need to add naps when sleeping polyphasically. The reduced light sleep doesn’t allow us to sleep as long and remain awake for as long as on monophasic sleep.
Comparison with SWS
Also, there is another important thing to talk about: Sleep spindles and K-complexes. Both these components appear both in light sleep and SWS; additionally, reducing these by too much can lead to the development of schizophrenia-type symptoms.
So far, these symptoms have not been present on a schedule with no SWS reduction. In other words, out of everyone that has adapted to a polyphasic schedule, no one has developed these symptoms. We actually have one case that developed schizophrenia-type symptoms from a polyphasic schedule; however, it was because they stayed on the Tesla schedule for several months. Tesla schedule is not recommended for average sleepers. It is even extreme for sleep mutants.
Debunking sleep architecture
To find evidence for in order to make the claim that polyphasic sleep is dangerous, what questions does it take to answer? Regarding sleep architecture:
- SWS and REM durations decrease after adapting to a polyphasic schedule.
- Reducing SWS and REM definitely leads to negative health effects.
- Cutting light sleep leads to negative health effects.
